Anaesthetics, Airway
AIRWAY ASSESSMENT
A difficult airway may present as difficult ventilation, difficult laryngoscopy, difficult intubation or a combination of these. 30 - 40% of anaesthetic related deaths are due to the inability to manage the airway, resulting in hypoxia. The definition of difficult intubation is greater than 3 attempts at intubation, or greater than 10 minutes of attempted intubation. The incidence of difficult intubation is about 0.5 - 16.6% (the rate varies depending on the definition). 15% of difficult intubations were also associated with difficult mask ventilation.
Successful airway management ensure adequate tissue oxygenation. Most airway related deaths and morbidity result from a failure to ventilate and oxygenate rather than a failure to intubate. It is important for the anaesthetist to be skilled at airway management without tracheal intubation.
Facemask ventilation
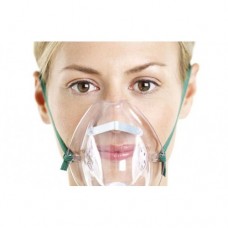
Anaesthetic facemasks are designed to fit the contours of the face with minimal pressure. They are cushioned to minimize the leakage of gases and come in different sizes. The correct size for the patient will minimize dead space and provide a good seal. Paediatric masks can be cushioned circular masks or the Rendell-Baker mask, which is designed to minimize dead space.
Once the patient loses consciousness in the supine position, the tongue and epiglottis fall towards the posterior pharyngeal wall tending to obstruct the upper airway. The anaesthetist can perform chin lift and jaw thrust manoeuvres to open the airway. The facemask is held onto the face using the thumb at the bridge of the nose, fifth finger behind the angle of the mandible and the rest of the fingers pull the mandible into the mask. The mask should not be pushed onto the face. Edentulous patients and beards will make it difficult to achieve an adequate seal with a facemask for positive pressure ventilation.
Pharyngeal airways
Pharyngeal airways relieve upper airway obstruction caused by soft tissue relaxation during unconsciousness. They are able to separate the soft tissues from the posterior pharyngeal wall. Insertion will require attenuation of the upper airway reflexes to prevent regurgitation, gagging and laryngospasm. Measuring the distance from the tragus of the ear to the corner of the mouth allow the anaesthetist to choose the correct size of an oral airway.
Laryngeal mask airway
The LMA consists of an elliptical bowl-shaped mask that sits over the laryngeal inlet surrounded by a cuffed rim. There is a tubular portion that sits in the oropharynx and mouth. It can be connected to the breathing circuit. It is available in adult and paediatric sizes and there is now a version with a gastric lumen that sits in the upper oesophagus to reduce the risk of regurgitation into the larynx (ProSeal). A reinforced version is also available.
Hfoc High Flow Oxygen Conserver
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT HFOC HI..
$764.50 Ex Tax: $695.00
Incentive Spirometer 3 Ball Sureflow
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$35.00 Ex Tax: $35.00
Key Ring Resus Mask Cpr Resuscitation Face Shield X 1 (Green Nylon Bag)
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$6.00 Ex Tax: $6.00
Key Ring Resus Mask Cpr Resuscitation Face Shield X 1 (Green Nylon Bag) (Free Postage)
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$15.00 Ex Tax: $15.00
Laerdal Compact Suction Pump Unit 4 300ml Or 800ml
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT LAERDAL..
$1,089.00 Ex Tax: $990.00
Laerdal Little Anne CPR Manikin Replacement Airways
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$6.60 Ex Tax: $6.00
Laerdal Suction Pump Unit Hospital Or Remotely
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT LAERDAL..
$4,125.00 Ex Tax: $3,750.00
Laryngoscope Disposable Blades & Handle Macintosh Type All Sizes
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$33.00 Ex Tax: $30.00
Liberty 7e-a Portable Suction Pump 18 Litre Oil Free Low Noise Tga Approved
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$544.50 Ex Tax: $495.00
Liberty 7e-a Portable Suction Pump 18 Litre Oil Free Low Noise Tga Approved (Free Postage)
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$660.00 Ex Tax: $600.00
Liberty Bestneb High Performance Pump & Accessories
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$270.00 Ex Tax: $270.00
Liberty Bestneb High Performance Pump & Accessories (Free Postage Item)
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$285.00 Ex Tax: $285.00
Liberty Nebuliser Pump Filters 5 Pack
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$16.50 Ex Tax: $15.00
Liberty Nebuliser Pump Nebulizer Compact Compressor Medical Asthma Hospital
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$185.00 Ex Tax: $185.00
Liberty Nebuliser Pump Nebulizer Compact Compressor Medical Asthma Hospital (FREE POSTAGE)
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$200.00 Ex Tax: $200.00
Nasal Oxygen Cannula With Nasal Prongs (Adult)
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$3.00 Ex Tax: $3.00
Nasal Oxygen Cannula With Nasal Prongs (Child)
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$3.00 Ex Tax: $3.00
Nasal Oxygen Cannula With Nasal Prongs (Neonate)
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$3.00 Ex Tax: $3.00
Nebulizer Mask Adult Complete With Accessories
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$8.00 Ex Tax: $8.00
Nebulizer Mask Adult Complete With Accessories (Free Postage)
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$20.00 Ex Tax: $20.00
Nebulizer Mask Child Complete With Accessories
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$8.00 Ex Tax: $8.00
Nebulizer Mask Child Complete With Accessories (Free Postage)
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$20.00 Ex Tax: $20.00
Oxygen Mask With 210cm Tubing (Free Postage)
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$23.00 Ex Tax: $23.00
Oxygen Mask With 210cm Tubing Adult
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$10.00 Ex Tax: $10.00
Oxygen Mask With 210cm Tubing Child
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$4.00 Ex Tax: $4.00
Oxygen Mask With 210cm Tubing Child (Free Postage)
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$18.00 Ex Tax: $18.00
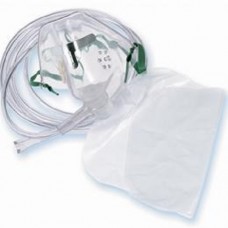
Oxygen Mask With Non Rebreat her Bag With 2 Metre Tubing
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$10.00 Ex Tax: $10.00
Peak Flow Meter E-Chamber Personal Monitoring Device Respiratory Asthma
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$25.00 Ex Tax: $25.00
Peak Flow Meter For Asthma Respiratory Patients Child
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$30.00 Ex Tax: $30.00
Portable Nebuliser e-chamber
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$155.00 Ex Tax: $155.00
Respi Flow Fs Incentive Exerciser Tri Ball Spirometer
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT RESPI..
$30.80 Ex Tax: $28.00
Respi Flow Fs Incentive Exerciser Tri Ball Spirometer (Free Postage)
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT RESPI..
$41.80 Ex Tax: $38.00
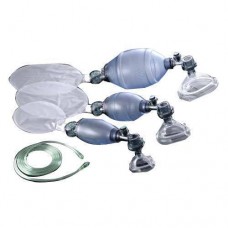
Resuscitator Adult Disposable With Mask Tubing Bag & Safety Pop-off Valve X 1
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT Resus..
$40.00 Ex Tax: $40.00
Resuscitator Child Disposable With Mask Tubing Bag & Safety Pop-off Valve X 1
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT Resus..
$40.00 Ex Tax: $40.00
Resuscitator Infant Disposable With Mask Tubing Bag & Safety Pop-off Valve X 1
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT Resus..
$40.00 Ex Tax: $40.00
Sale On Now Airphysio Mucus Removal Lung Expansion Device Natural Breathing Aid Air Physio
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT AirPh..
$88.00 Ex Tax: $80.00
Spacer La Grande Anti Static 510ml Large Spacer e-Chamber
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$20.00 Ex Tax: $20.00
Spacer La Petite Anti Static 220ml Spacer e-Chamber
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$18.00 Ex Tax: $18.00
Spacer La Petite With Small Mask Anti Static 220ml e-Chamber 0-6 Ages
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$25.00 Ex Tax: $25.00
Spacer Large Mask For Adults & Older Children e- Chamber Boxed
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$10.00 Ex Tax: $10.00
Spacer Small Mask For Infants & Children e- Chamber Boxed
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$10.00 Ex Tax: $10.00
Spacer Turbo Anti Static 220ml Spacer e-Chamber Blister Pack
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$18.70 Ex Tax: $17.00
Spacer Turbo Anti Static 220ml Spacer e-Chamber Blister Pack
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$15.00 Ex Tax: $15.00
Spare Filters To Suit Liberty Bestneb Nebuliser High Performance 5/pkt
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT FILTE..
$16.50 Ex Tax: $15.00
Suction Tube 3 Meters Double Wrap Sterile ORNEX510
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$5.50 Ex Tax: $5.00
Tracheostomy Vent T Portex 100/570/015
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$15.00 Ex Tax: $15.00
Vacuum Pump Manual Ferno Quality Portable Suction Pump
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT VACUUM ..
$242.00 Ex Tax: $220.00
Volumatic Spacer
SOLUTIONS MEDICAL PROVIDES QUALITY MEDICAL SUPPLIES DEVICES & EQUIPMENT ..
$18.70 Ex Tax: $17.00

 AUSTRALIA-WIDE SHIPPING $15
AUSTRALIA-WIDE SHIPPING $15



















-228x228.jpg)
-228x228.jpg)








